Starting a new summer with a new knee: My experience having a total knee replacement surgery
By Catherine Miller

In spring of 2022 I visited an orthopedist due to recurring knee pain thinking I needed a minor surgical meniscus repair. After an hour and a couple of X-rays I was told that the meniscus was not the issue. I had osteoarthritis and would eventually need a total knee replacement.
They would begin to treat me conservatively to postpone surgery. After all, I’m in my 50s and knee replacements are for old people, right?
We tried physical therapy and pain medication. The pain progressed and I could barely walk. Cortisone shots were tried with little relief. Finally, my surgeon agreed that I was a current candidate for total knee replacement surgery, despite my young(ish) age. As we talked about scheduling the surgery I was told the earliest date was nearly eight months away!
Apparently, our post-pandemic medical world left a backlog of people waiting for elective surgeries. While knee replacement is technically an elective surgery, my pain had increased quickly and it seemed pretty mandatory to me.
While I knew I was in capable hands with my first surgeon, I decided to seek a second opinion to see if I could shorten that wait.
We are fortunate in our area to have an abundance of great orthopedists in our midst. Taking the recommendation of a friend I transferred my care to orthopedic surgeon Keith Stube of the Western New York Knee Center.

Stube not only had a surgery date months sooner, but also recommended gel shots which would give me relief while awaiting surgery. Done. I scheduled surgery and changed my physical therapy regimen from conservative treatment to pre-operative treatment.
“The focus when conservatively managing knee pain is on reducing pain and inflammation to allow patients to return to moving around more comfortably,” said physical therapist Bernard J. Ryan, owner of Ascend Physical Therapy, “Once a candidate for a total knee arthroplasty, the emphasis shifts more toward strengthening and range of motion to maximize mobility and strength heading into the surgery.”
As Ryan told me, performing daily exercises to gain strength and motion is important. So that is what I focused on, right up until the day of surgery.
“The stronger you are going into surgery, the stronger you’ll be coming out of the surgery!” he said.
The following are things I was not aware of prior to considering a total knee replacement surgery:
You will likely go home the day of your surgery
My surgery was at 11 a.m. I was home by 7 p.m. I had to hit the “markers” before being allowed to leave the hospital, namely walking a few steps with a walker, climbing a few stairs, etc. Once done, I was sent home with a notebook of information and all necessary medications. I was tired, nauseous and grateful to be home.
Stube called me a few hours later to check on my condition. I felt more than comfortable being back home knowing I still had medical oversight.
Physical therapy will start immediately after surgery
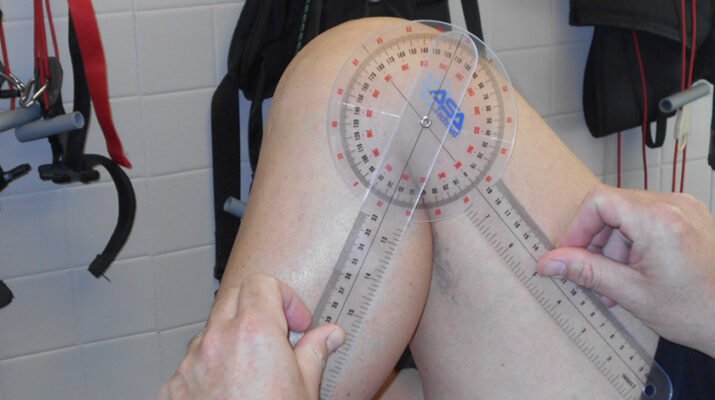
My first visit to PT was two days after surgery. The toughest part was bending my knee to get into the car. Once there Ryan took measurements of the extension and bend of my surgical knee. While I was able to fully extend the leg, my bend was limited and painful. As Ryan said, “Regaining range of motion and working through stiffness after surgery can be difficult. It becomes paramount to break down scar tissue and adhesions to gain full flexibility of the knee early on post operatively.”
During PT my rehab team monitored progress and shared milestones with my surgical team.
Keep ahead of the pain
This was suggested by two family members who also had surgeries. Keep a list of medications and times taken. Keep up on pain meds, as well as laxatives to keep yourself comfortable. And ice ice baby! Elevation and icing the knee are pretty much what your world revolves around at the onset. Keeping the swelling at bay allows you to walk more each day. Remember, a new knee is a prothesis and your body is in repair mode.
Do your homework. But not too much
Your medical team has done this before. Ask them about what to expect as they are the best providers of medical information.
My surgical facility called me prior to surgery to tell me what medical equipment would be sent home with me (a walker and an ice machine) and what other items may come in handy (a shower chair and cane). They provided additional information when I pre-registered. A quick search on the internet provided additional insight on total knee replacements and contained blogs and support groups where post-surgical patients shared their stories.
While some of this proved useful, the caveat was that some of the internet information is not relevant to your situation or indicative of your experience. It’s best to get medical information from medical providers.
After two months I was ready to return to work. There had been many sleepless nights (which is common post-surgery) and times when I felt I was taking two steps forward and one step back, but I finally felt I was moving forward with recovery.
Stairs were still challenging, but my range of motion was great and I still continue my daily exercises. The best part is that the pain that was there every step I took last summer is now gone.
It was a long post-surgical period but definitely worth it. I attribute much of my knee replacement success to Stube and his group, the surgical team at Millard Fillmore Suburban Hospital and the folks at Ascend Physical Therapy. Thanks to them I have a more mobile summer to look forward to.
 Catherine Miller is a contributing writer for In Good Health magazine. She lives in Buffalo and has been a freelance writer in the WNY area for over twelve years.
Catherine Miller is a contributing writer for In Good Health magazine. She lives in Buffalo and has been a freelance writer in the WNY area for over twelve years.